The Virtual Lab: How VR & AI Are Transforming the Pharmaceutical Industry
AI and VR are driving innovation in drug research through to commercialisation and ensuring better treatment outcomes.
In an interview with BARMER, discover the groundbreaking possibilities of Virtual Reality in medical education for health care.
In recent years, advancements in eXtended Reality (XR) technologies, including Virtual and Augmented Reality, have created innovative human-computer interfaces that increasingly resemble natural human movements, interactions, and experiences.
Given the increasing complexity of medical procedures and tasks, and the time constraints on trainees' work, the field of medical science has a need for tools that accelerate learning and improve the lifelikeness of training. New XR and other simulation technologies are increasingly used in medical education and allow for more interactivity, immersion, and safety in medical training.
In a conversation with Digital Coordinator Maria Hinz from BARMER, one of the largest health insurers in Germany, we learn exciting insights into the topic of recognizing the potential and challenges of Virtual Reality Training in healthcare.
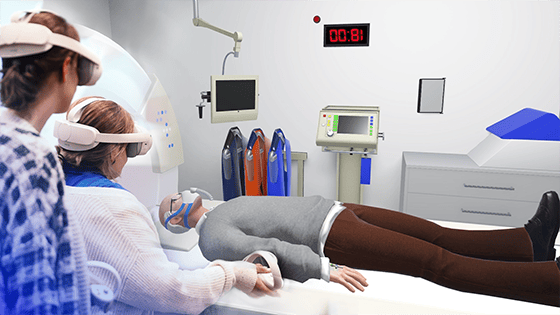
MH: Operations can be repeated as often as desired in virtual worlds. Errors can be identified, analyzed and eliminated. At the same time, we relive the interventions as realistically as possible – in an environment and with background noises that are very close to the actual situation. Surgeries can be trained as if you actually were holding the scalpel in your hand. This applies not only to surgeons, of course, but also to other professionals such as nursing staff or rescue workers. Through VR simulations, they can train rare or complex cases and thus improve their skills without taking risks for patients. In addition, VR simulations can also be used to prepare for medical emergencies or disasters.
VR also becomes interesting in the treatment of phobias and mental disorders such as anxiety and post-traumatic stress disorder (PTSD). Patients can be confronted with their fears in a controlled and safe environment in order to overcome them. This also works in a positive sense, incidentally also with animals. For example, cows that are shown a lush green meadow in the virtual world are said to give more milk.
Similarly, a suitable virtual environment can draw the attention of patients and reduce pain through distraction.
By working together via remote medicine, medical professionals and patients communicate better with each other. For example, if the GP and specialist and a patient are connected together, the X-ray images can be viewed again during the conversation or the heart rate displayed live. Nothing is unthinkable.
Virtual worlds are also a great place to exercise or relax. Therefore, VR can also be used to promote a healthy lifestyle by offering patients interactive exercises on the beach, in the mountains or in a spa.
Overall, VR offers great potential for healthcare to improve the effectiveness and efficiency of medical care and provide a better experience for all involved.
MH: Let's assume that the electronic patient file already contains other functionalities. Now imagine that you could not only view your health data on your mobile phone, but also see them tidied up and perfectly processed in a virtual world. The electronic patient file could be a walk-in room in which you could see your laboratory reports interactively processed in the future and your doctor's letters would fly chronologically ordered from the bookshelf to your desk, where you could read the most important aspects directly marked. Perhaps you could even walk through your treatment history together with a doctor to provide the best possible view of your situation.
Your health data can be displayed as virtual objects in one of these virtual environments, providing a visual representation of the data. Take a look at the chart of your blood glucose values displayed as a 3D object and explore it interactively. Perhaps directly together with your Diabetologist, even though they are sitting many miles apart in other rooms.
In combination with artificial intelligence, it would even be possible for doctors or nurses to interactively get a picture of the state of health and have the AI calculate how therapies and treatments will work.
Using VR environments, patients can better understand their health data previously collected in the electronic patient file and become more engaged with their own health.
MH: Introducing Virtual Reality into nursing and medical care may raise concerns among some patients that the technology could interfere with the personal aspect of care. From my point of view, there are several ways in which healthcare actors, including health insurers and clinics, can alleviate patients' fears.
First of all, it is important to explain what VR is and how it is used in (health) care. This is not about the usual academic technical texts but about simple explanations with a storytelling that covers the individual situations and needs of the patients. Transparency is very important here to convey a positive feeling. When we as a health insurance company deal with future technologies, we see them as a support for professionals, not as a substitute. So we have to ensure and also emphasize in communication that VR supports care and nursing, but does not replace the relationship between patients and medical staff. This applies to VR as well as to the use of artificial intelligence. The best way for new technologies to work is in collaboration with professionals. If these technologies are developed with a meaningful ethical compass, they can also be highly inclusive. For example, in treating stigmatized medical conditions or for people who would not be able to visit a doctor without mobile barriers.
Clinics can also ultimately seek feedback from patients to ensure that VR is being used effectively and that everyone's needs and preferences are being taken into account. Regular evaluations can ensure that VR is used as a complement to care and not as a substitute for face-to-face contact.
Overall, VR offers great potential for healthcare to improve healthcare effectiveness and efficiency providing a better experience for all stakeholders.
MH: Digitisation is progressing very slowly in the health sector. There are various reasons for this. Health data receives the highest level of protection. Processing accordingly requires special security measures to ensure the confidentiality and integrity of this data. Digital tools must therefore meet the high data protection requirements on the one hand and still be intuitively usable on the other. To resolve this conflict of goals, data protectors, legislators and developers must work well together.
Once we have user-friendly applications that optimally guarantee data protection, another question emerges – that of interoperability. The various digital applications in the health sector must be compatible with each other to enable a smooth exchange of information between clinics, health insurers and other actors. Uniform standards and interfaces must be defined for this.
At BARMER, we are currently focusing on the topic of digital competence - both internally and externally. We see that the acceptance of digital services is closely linked to technical competence and familiarity with the technology. It is therefore important that insured persons and healthcare staff are sufficiently trained to be able to use digital tools effectively. A basis for this has been created with the possibility of providing benefits for the acquisition of digital health skills.
In addition to the regulatory and data protection challenges, ethical questions beyond the generally applicable legislation will always arise. As BARMER, we are the first health insurance company in Germany to actively address the issue of corporate digital responsibility and publish an annual CDR report. For all future issues that are not yet regulated by law, we have developed values with scientific support. These help us to find answers to such future questions. Thus, we can also clearly state that sovereignty and solidarity are very important to us and that we therefore support voluntary data donation. Similar ethical discourses must also be conducted in public in order to enable sovereign opinions of empowered patients in the first place on the basis of transparent information and a fundamental understanding of technology.
Thank you very much, dear Maria, for this interesting conversation!

Digital transformation and communication expert Maria Hinz, is more than ten years working in the internet-driven world of business, associations and politics. She is passionate about responsible digitalization and strives for excellence and innovation in the healthcare of the future. Maria Hinz inspires through authentic female leadership and empowers people by making complex issues tangible.

AI and VR are driving innovation in drug research through to commercialisation and ensuring better treatment outcomes.
How the BARMER Hub uses Virtual Reality for the onboarding of international employees from abroad for smooth integration.
VR in medicine: Learn how the digitization revolutionizes the healthcare industry and how Virtual Rreality helps to improve the education of...
Stay up to date on new insights in VR / AR learning with AI and build or improve your knowledge within the technology.